Short-Term Association between Sulfur Dioxide and Mortality: A Multicountry Analysis in 399 Cities
Resumen
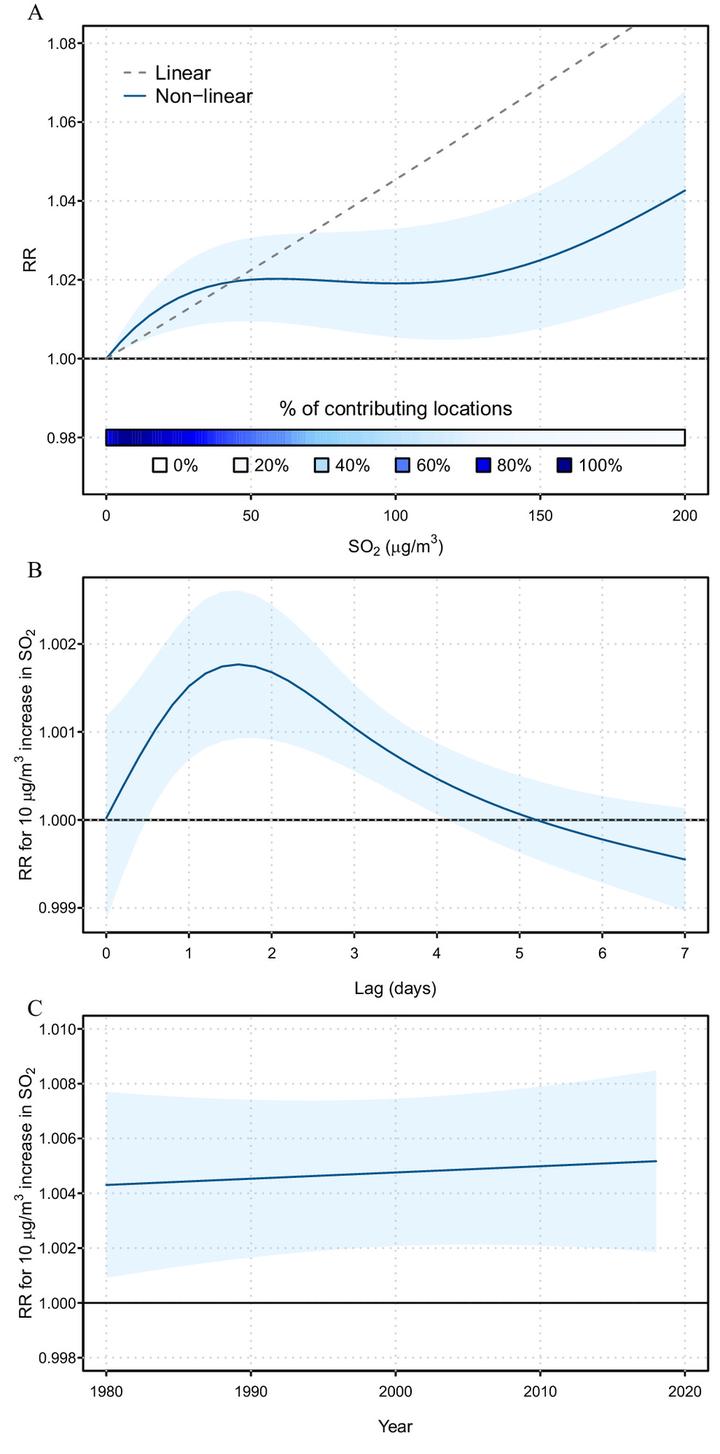
Background: Epidemiological evidence on the health risks of sulfur dioxide (SO2) is more limited compared with other pollutants, and doubts remain on several aspects, such as the form of the exposure-response relationship, the potential role of copollutants, as well as the actual risk at low concentrations and possible temporal variation in risks. Objectives: Our aim was to assess the short-term association between exposure to SO2 and daily mortality in a large multilocation data set, using advanced study designs and statistical techniques. Methods: The analysis included 43,729,018 deaths that occurred in 399 cities within 23 countries between 1980 and 2018. A two-stage design was applied to assess the association between the daily concentration of SO2 and mortality counts, including first-stage time-series regressions and second-stage multilevel random-effect meta-analyses. Secondary analyses assessed the exposure-response shape and the lag structure using spline terms and distributed lag models, respectively, and temporal variations in risk using a longitudinal meta-regression. Bi-pollutant models were applied to examine confounding effects of particulate matter with an aerodynamic diameter of ≤10μm (PM10) and 2.5μm (PM2.5), ozone, nitrogen dioxide, and carbon monoxide. Associations were reported as relative risks (RRs) and fractions of excess deaths. Results: The average daily concentration of SO2 across the 399 cities was 11.7 μg/m3, with 4.7% of days above the World Health Organization (WHO) guideline limit (40 μg/m3, 24-h average), although the exceedances occurred predominantly in specific locations. Exposure levels decreased considerably during the study period, from an average concentration of 19.0 μg/m3 in 1980-1989 to 6.3 μg/m3 in 2010-2018. For all locations combined, a 10-μg/m3 increase in daily SO2 was associated with an RR of mortality of 1.0045 [95% confidence interval (CI): 1.0019, 1.0070], with the risk being stable over time but with substantial between-country heterogeneity. Short-term exposure to SO2 was associated with an excess mortality fraction of 0.50% [95% empirical CI (eCI): 0.42%, 0.57%] in the 399 cities, although decreasing from 0.74% (0.61%, 0.85%) in 1980-1989 to 0.37% (0.27%, 0.47%) in 2010-2018. There was some evidence of nonlinearity, with a steep exposure-response relationship at low concentrations and the risk attenuating at higher levels. The relevant lag window was 0-3 d. Significant positive associations remained after controlling for other pollutants. Discussion: The analysis revealed independent mortality risks associated with short-term exposure to SO2, with no evidence of a threshold. Levels below the current WHO guidelines for 24-h averages were still associated with substantial excess mortality, indicating the potential benefits of stricter air quality standards.